One aspect of the original outbreak of coronavirus in March and April that has not received enough attention was the spread of the virus in NHS hospitals. With NHS staff lacking Personal Protective Equipment – and as we know now, suffering from a lack of preparedness – the virus spread at rapid speed between people in close proximity in hospitals – the very places where people expected to get better, not worse.
In this first phase of the pandemic at least one in eight patients contracted the virus while already in hospital. These patients tended to be older and frailer, and if they survived, they ended up staying in hospital on average for more than a month.
On 24 June, all NHS Trusts and Foundation Trusts were required by NHS England to apply the UK recommended Infection Prevention and Control Guidance more robustly. This meant all hospital staff wearing surgical face masks irrespective of the setting, and visitors and outpatients wearing a form of face covering.
Over the summer the spread of the virus in hospitals fortunately reduced. Until now, that is.
NHS England publishes a daily Covid ‘situation report’ that gives the number of new hospital cases and breaks down how many came from care homes and how many are from wider society, which they term the ‘community’. In line with NHS England guidance, patients who test positive after seven days or more in hospital are considered probable healthcare-associated infections (HCAIs).
We noticed that in some of the larger hospital trusts, the amount of absentee staff for Covid-19 has been steady throughout the summer and autumn, indicating likely low-level transmission among staff. But, among patients it is a different story. The current rate of infections in a healthcare setting is hovering at around 20 per cent, up from 12 per cent in October.
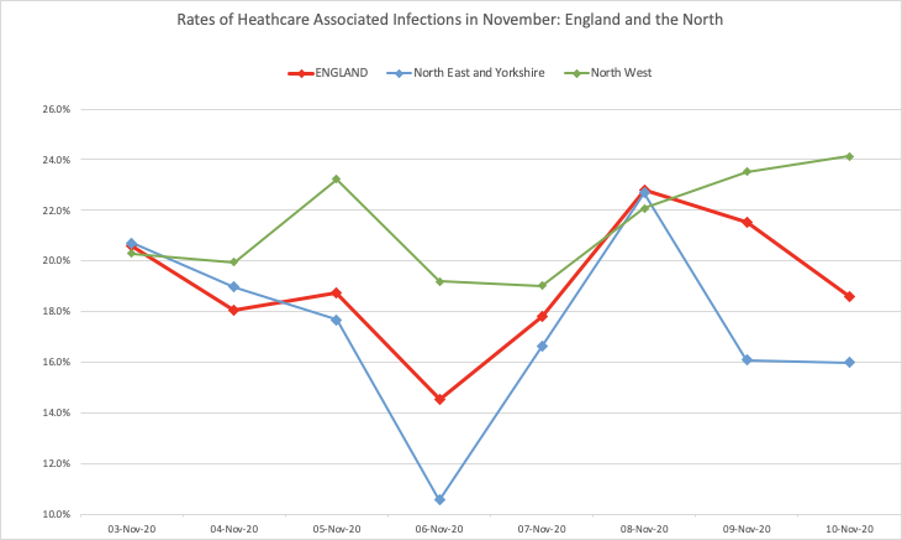
This figure is starker in particular regions. In the North West, for instance, it is as high as 24 per cent, up from 13 per cent at the beginning of October.
Sharp rises in hospital infections can occur through a variety of mechanisms: sometimes an unexpected positive case comes up in a non-infectious part of the hospital, and other patients are identified; while some outbreaks occur when staff are found to be positive on screening. There are instances where staff have come to work with symptoms, and then turned out to be positive.
The problem, though, is widespread across the UK: we identified eleven reports of major outbreaks in healthcare settings during October. In Wales, there were 192 cases linked to a hospital outbreak, with 12 confirmed deaths linked to an outbreak in the Cwm Taf Morgannwg health board area. Politicians have demanded a probe into outbreaks at the board’s hospitals after 57 deaths were related to hospital outbreaks.
In Scotland, up to four people died after a Covid-19 outbreak on a cancer ward in an Edinburgh hospital.
In England, South Tees Hospital Trust has had seven separate outbreaks of Covid-19. An inquiry was launched in Tameside after in a small district hospital more than a third of all coronavirus deaths among inpatients in England occurred in a week; 150 patients were infected by Covid-19 in University Hospitals Bristol and Weston Foundation Trust – and a third died.
Covid is an extremely difficult infection to manage in enclosed spaces that are not purpose-built for pandemics. The NHS estate is largely suited to high volume elective care and not infectious outbreaks.
Public Health England’s Infection prevention guidance depends on creating designated areas within Emergency/Research Resuscitation Departments and establishing the separation of patient pathways and staff flow to minimise contact between pathways. The current structure of many hospitals, however, makes this near impossible.
An in-depth report of an outbreak at St. Augustine’s Hospital, Durban, South Africa identified a lack of separation of Covid-infected patients from other patients, likely stemming from the Emergency Room. It resulted in 15 patients dying. A lack of suspicion and awareness of the threat, together with frequent movement of patients inside the hospital contributed to the swift spread of the virus.
Covid-19 and all other hospital infections are not easy to control, the current NHS facilities are not fit for purpose, and rates of acquired infections are adding considerable numbers – about 20 percent – to those in hospital beds with Covid.
We must assess whether the use of dedicated areas and the other measures will be sufficient. If they are not, the only way to control these outbreaks is to separate hospitals.
The causes of hospital-acquired infection are complex – it will not be easy to sort. We’re in this for the long term and the sooner we start analysing the problem the sooner we will find solutions.







Comments