As a result of a ruptured appendix, I am infertile. The appendicitis was followed by gangrene and peritonitis, which permanently blocked my fallopian tubes and left me having to do IVF for a chance to have my own child.
I have never felt shame about my situation but I have felt isolation and grief, both of which would be very much more bear-able if people were prepared to talk openly about in-vitro fertilisation — to dispel the taboo that still surrounds it.
IVF in its various forms is incredibly common these days. More than 2.5 million babies born in the past seven years began their life in a Petri dish. For various reasons, some known, some unknown, overall birth rates in the West are falling rapidly and infertility is rising: pretty soon as many as one in every ten children born in this country will owe its life to fertility treatment.
You might reasonably think, then, that when I underwent my first (failed) IVF cycle, I’d have been surrounded by friends and acquaintances keen to give advice and share their experiences with me. The truth is that I struggled to find any, and when I raised the subject in public people either shifted uncomfortably — as though I had transgressed a social boundary — or reacted with fascination, wanting to know all the ins and outs.
Everyone I spoke to knew someone who had been through it, but no one would admit to having done IVF themselves. One couple I met at a dinner party knew intimate details of a ‘friend’s’ treatment that they were only too willing to share. When I later discovered this same couple had non-identical twins, their expertise suddenly made sense. They did subsequently own up but I was disheartened that they’d been so coy at first.
To a certain extent, I understand all this reluctance to talk about IVF. Back in the 1980s when the first ‘test-tube babies’ were being born, patients were under pressure to keep their treatment secret. The receptionist at the pioneering Bourn Hall Clinic, Vivien Collins, has spoken of women expressing disgust that she worked in a ‘test centre where they made babies’. And that horrified reaction, the idea that IVF involves some sinister process, still lingers today.
Last spring the designers Domenico Dolce and Stefano Gabbana branded IVF children ‘synthetic’, which provoked a public spat with Elton John. For most people of my parents’ generation, IVF is an unknown and therefore alarming.
The other reason for keeping schtum is superstition. Couples feel that if they talk about their hopes, they may not come true. And even if all goes well, having a IVF friend can be hard. It might seem sensible to buddy up with another patient in the clinic, to share the ups and downs, the trials of nightly injections and invasive scans — but statistically only one woman in three will end up with a baby at the end of the agonising process. How do you commiserate with your pal or continue a friendship when you’re no longer in the same boat? So women in fertility-clinic waiting rooms traditionally stare down at their iPads and stalk fertility forums looking for advice, rather than turn to those beside them.
A warning to anyone thinking of IVF: there’s something both glutinous and ghoulish about those fertility forums. It’s a euphemistic world where the language of relationships is infantilised and creepy acronyms are universally adopted. There are no boyfriends or husbands, only ‘DH’ (dear husband) for even the most useless man. Rather than being wished luck, you are ‘sent babydust’ and women’s tales of miscarriage are peppered with tragicomic flying-baby emoticons. You must navigate your way through the BFNs and the BFPs (that’s big fat negative and big fat positive) and my personal favourite BD (baby dance — yes, that’s sexual intercourse) to try to make sense of your experience.
The forums make me wish all the more that we could, as a society, talk openly and sensibly about infertility. The women online are clearly tough: they’ve endured numerous, arduous treatment cycles, not to mention miscarriages. Yet online they communicate in the written equivalent of baby voices. We do everyone a disservice by being coy.
If we talked about it more, we’d all know that fertility treatment isn’t the preserve of the spoiled, rich or vain — it’s available on the NHS and rightly so. With fewer people able to buy a home in their twenties, more women working and life expectancy increasing, it’s only going to get more common for women to have children later in life. And as mothers get older and treatment more effective and cheaper, the ratio of assisted to natural births is only going to narrow. We should be teaching our daughters not just how to avoid getting pregnant, but what to do if they can’t conceive. It would help women plan their families better if girls knew from the start about all the difficulties of a late-in-life pregnancy.
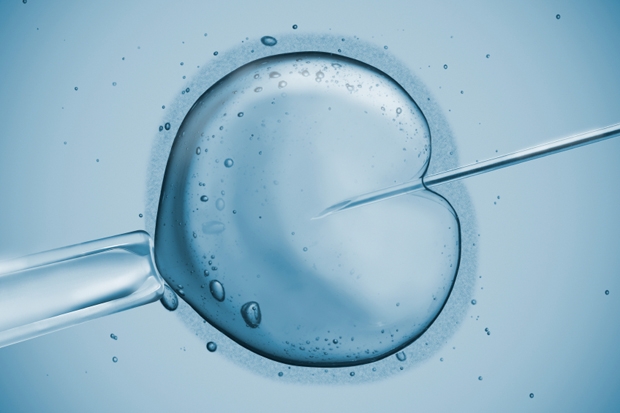
Because of the stigma still hovering over IVF, the science is moving faster than public awareness, and this is dangerous as well as unnecessary. Many IVF clinics are now offering both ICSI (intracytoplasmic sperm injection, which means the doctors can select a healthy-looking sperm) and genetic screening. But we just don’t know how safe either of these procedures are, or whether they’re more likely to lead to babies with birth defects. The frontier children are only just reaching adulthood and studies into potential health risks remain inconclusive. If the public were informed and interested, they’d be pushing for the NHS to fund rigorous studies and hold unscrupulous clinics to account.
There should be no shame at all in having an IVF baby, or in undergoing IVF. The children born of IVF are meticulously planned for and warmly welcomed, more so than any ‘Oops, the condom split’ baby. If I’m ever lucky enough to have a child, and to find myself in receipt of those awkward questions about reproduction that every mother is asked, I’m going to tell my child the truth about how they came to be, because they should be proud.





Comments