When my unborn baby was a five-month-old fetus, twisting about in the internal dark, he was given a death sentence by a man I shall call Anton.
We’d gone, my husband and I, for a 20-week scan at our local hospital. Anton was our designated sonographer; we arrived in his room bright-eyed and anxious, as even elderly first-time parents are. We looked to Anton for reassurance, but Anton looked only at his assistant, a sulky 19-year-old sexpot from Romania.
The sexpot tried seven times to dig into the vein in my right arm, then began on the left. ‘Don’t worry, good practice, try again,’ said Anton to her, kindly. ‘No, don’t worry at all!’ said I, pathetically.
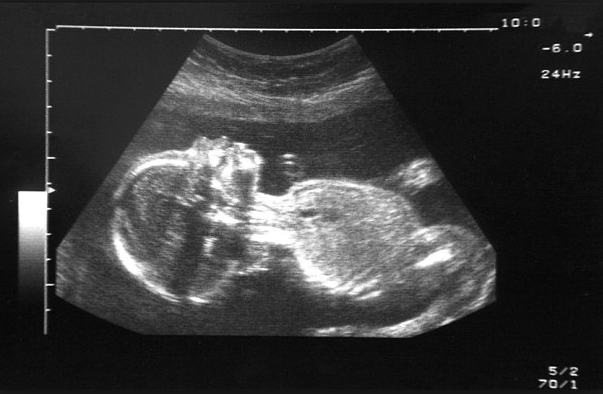
During an ultrasound the sonographer runs a plastic scanner over the mother’s naked belly, and that classic grainy image of the fetus appears on screen. For Anton, this was a romantic opportunity. The hottie held the mouse — ‘She is learning the ropes’ — Anton placed his mitt over hers and together their hands glided over my belly, circling, swooping in the manner of Torvill and Dean. ‘Spine, kidneys…’ Anton whispered lovingly in her right ear, ‘head circumference, abdomen, femur…’ Can we find out the baby’s gender? I asked. Is everything OK? Anton kept schtum. Why do some sonographers stay silent, when every parent they meet looks desperately to them for reassurance?
After half an hour Anton pronounced himself done and told us to take a seat. ‘Well. Baby is quite small,’ he began.
Is that a problem? I said, not panicking just yet. Still inhabiting what was soon to be our old reality, as parents-to-be of a healthy child.
‘In this case, I think yes,’ said Anton. ‘I think either genetic abnormality or more likely placental insufficiency.’ Did he turn to see if the hottie was admiring his confident diagnosis, or is that a spiteful reimagining?
And what does that mean?
‘It means,’ said Anton, ‘placenta is failing. Baby will not grow.’
Anton had three reasons to support his theory. The first was a discrepancy between the baby’s head size (normal) and his stomach (small). The second was a relatively new test, the ‘doppler’ scan of uterine arteries. ‘High resistance,’ said Anton. ‘Baby struggling.’ The third reason was the most surreal: ‘Deep placental legs,’ said Anton. Legs? ‘Yes. Legs.’ Legs? I asked again, pointing to my own.
‘No. Leks. Leks!’ said Anton crossly. ‘Like pools.’ Oh, Lakes, I see, I said, though I didn’t. I’ve been haunted ever since by visions of these mysterious lakes, full of pitchy, murderous water, enticing babies to their doom.
Anton’s eventual diagnosis, written like a death sentence across our scan notes, was: IUGR. Interuterine growth restriction (early onset). He did mention that only the fetal specialist could make a proper diagnosis, but the specialist wasn’t free for five days. Anton also made it plain he thought our child a write-off. ‘Do you still want to know the sex?’ he said as we fumbled silently into our coats. ‘Still’? Why ‘still’? I stared at him blankly. He shrugged. ‘Boy,’ he said and turned away.
As I understand it, sonographers receive no training in how to talk to anxious parents. Most, I’m sure, need none. Some like Anton definitely do. It was quite clear from the way he spoke that he assumed we’d bin this malformed kid and start again. This is basic misunderstanding of parent mentality. For most expectant parents, after five months of pregnancy, that grainy blob is definitely a child; their child. Inevitably, irrevocably, they love it. I remember the terrible moment, at about 18 weeks, when I realised I loved the unborn blob. I quaked at the implications.
This being a real baby, not just a potential one, after Anton’s prognosis, my husband and I began to mourn. We sat for an hour in the hospital corridor, watching the watercooler belch, feeling panic and despair, then in the end, resigned. That night I had two large glasses of red wine. The next morning I visited the church where my husband and I got married and lit a candle for the unborn boy.
Then, as is the way of the middle classes, I booked and went for a private scan with a professor of fetal medicine. £150 seemed a small price to pay to shorten the wait to see a specialist. After this second scan I realised the importance of making sure that Anton and his like have not just empathy training, but a proper understanding of the tests they perform — specifically how unreliable they are.
Same type of machine, same 20-week scan but this time a very different manner and, astonishingly to us, a different result: ‘Lovely spine, lovely abdomen, perfect… hmm. Let me see your diagnosis again,’ said the professor. ‘IUGR? Pah! I’m afraid you have a perfectly ordinary baby.’ He grinned. ‘You have a boring baby!’ Boring baby. Are there two more beautiful words?
Anton’s mistake, the professor explained, was false certainty. He’d doomed my baby on the basis of measurements he should have seen only as guidelines. ‘Your baby was upside down for the first scan. This means all the measurements get squashed,’ he said. ‘They are not to be trusted.’ Even if the baby had been right way up, the measurements and how they’re interpreted are approximate. The parameters for normality used in most NHS hospitals are based on studies from the 1970s.
The clincher for Anton had been the doppler scan measuring the arterial blood flow to the uterus. This is a newish test, the professor told me, and very useful but subject to false positives. What looks like a worrying result at 20 weeks often resolves itself later on. As for the awful placental lakes — they turn out to be as mythical as they sound. ‘40% of your placenta is leks,’ Anton told me. The professor could see none at all.
Antenatal departments are full of wonderful, warm, professional people, though I don’t count Anton among them. The NHS has a duty to them, and to parents, to train them to understand the tests they do: how robust each finding is, what margin for error exists.
As I write this, my son is stretching in the sunlight beside me — a living testament to the unreliability of scans. Two weeks old, small, sometimes cross, miraculously ordinary.






Comments